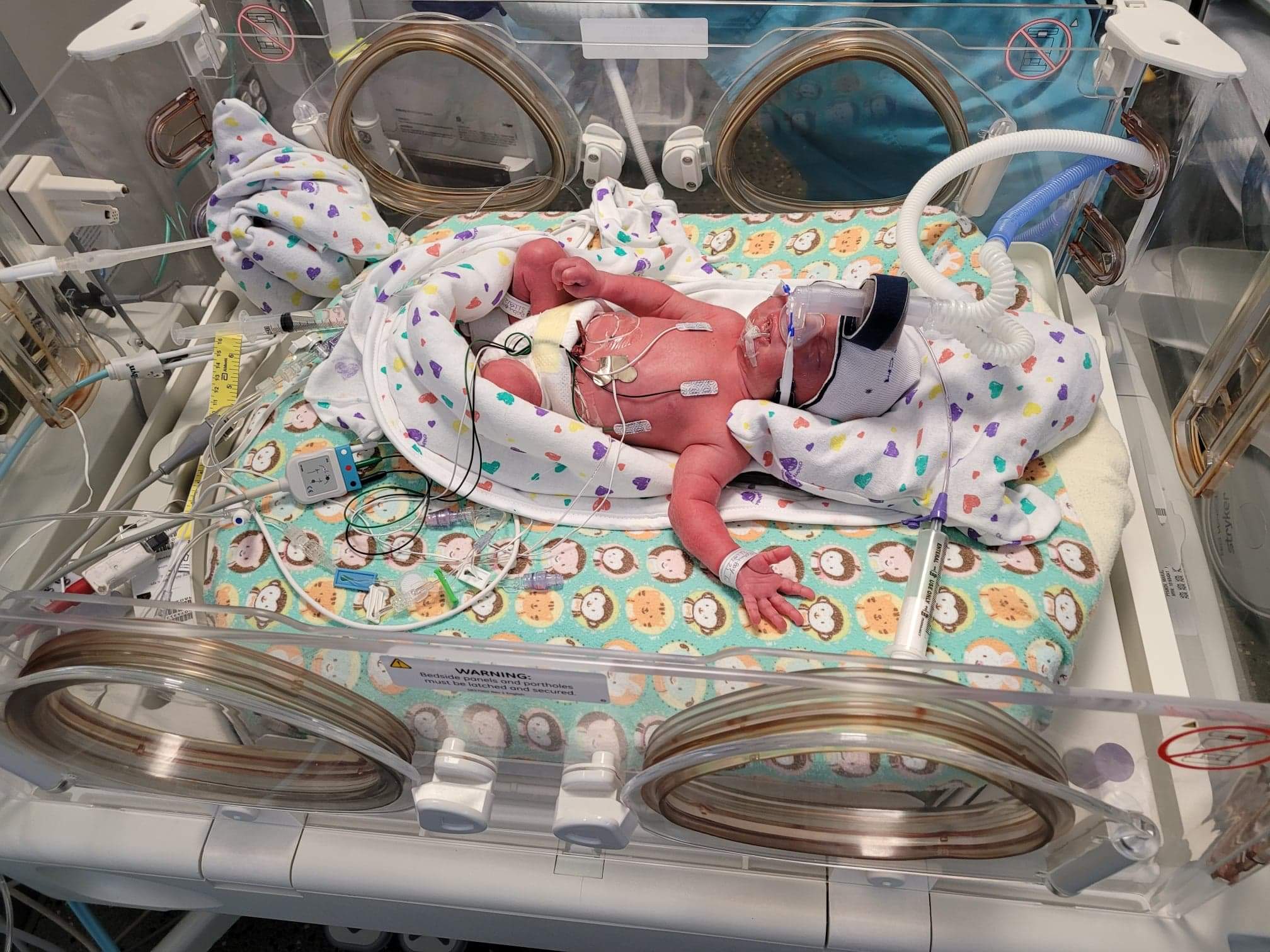
New babies bring excitement. However, that excitement can quickly turn to worry when you realize you’re facing a premature birth. What to expect with premature babies can be unknown to many of us.
While the worry remains, we can find a bit of relief in knowing we live in a time where modern medicine allows even the earliest preemies to have a chance of survival.
More than just survive, modern medicine also means many preemies thrive exceptionally well.
Premature Babies – What To Expect Week By Week
Each day of pregnancy impacts your baby’s development. Every baby born before 37 weeks is premature. However, a 25-week baby is very different than a 29- or 35-week baby.
So, what should you expect for your premature baby based their gestation at birth? Their breathing, feeding and growth patterns will vary based on their gestation at birth. Here’s what to expect week by week:
What Is A 23-24 Weeker NICU Stay Like?
We now live in a time where more than half of babies born at 23-24 weeks survive. While there is a large jump between 23- and 24-week survival rates, some of that is based upon which babies receive intervention.
Some hospital facilities only intervene at 24-weeks, while others begin at 23-weeks. This is typically related to which equipment they have access to and current policies. Baby’s weight can also determine the ability for intervention
There are some facilities which offer medical intervention at 22 weeks, though survival rates are still low.
A baby born at this gestation will weigh a bit over 500 grams (one pound). As a NICU parent, even in the US, you will start to use grams over pounds and ounces. Metric measurements are used in medical care.
Babies at 23-24 weeks gestation typically have a breathing tube and are supported by a ventilator. Eventually, some will graduate to continuous positive airway pressure therapy (CPAP mask).
A CPAP machine increases air pressure in your baby’s throat so that their airways don’t collapse when they breathe in. A nasal cannula would follow as your baby’s breathing becomes more stable and then no respiratory support before NICU discharge.
Long-Term Respiratory Support
Some babies will remain on a ventilator and eventually require a tracheotomy for long-term respiratory support at home. Some may go home on oxygen with a nasal cannula. This is common for micro preemies; babies born weighing less than 800 grams (1.75 pounds) or prior to 26 weeks gestation.
While most NICUs aim to have babies graduate without medical devices, for micro preemies, these devices allow them to safely go home when they are otherwise well.
The use of steroids or not before birth impacts the type of initial and ongoing respiratory support.
Babies born at this gestation can’t safely eat by mouth yet. They will have IV lines, often umbilical lines as well, placed to provide medicine, nutrition, and hydration. Some will have more long-term IV lines such as PICC line or midline.
Depending on how a baby is doing, they will eventually begin feeds via a feeding tube placed in their nose (NG) or mouth (OG).
Breast milk remains a biologically normal food as a mother’s milk is different than had she given birth to a full-term baby. At this gestation, however, many healthcare providers fortify breast milk with extra calories and nutrition which babies typically get in the third trimester.
Supporting micro preemies is a newer area of medicine and the evidence is still growing regarding the best way to help these tiny babies grow.
Micropreemies Going Home
Some babies will go home with no feeding support. They will be at the breast or feeding with a bottle. Others will go home with an NG tube (a feeding tube in the nose), or with a G or J tube (stomach or intestinal tubes) for long-term feeding support. Babies near their due date might use long-term feeding support. This happens if they have ongoing feeding complications.
It will be important to work with healthcare providers familiar with preemie development. All preemies, especially the earliest ones, benefit from long-term support with developmental pediatricians and a variety of therapists.
Sometimes this is to receive services, other times it’s simply to monitor preemie babies as they’re at an increased risk for developmental delays and chronic health conditions. Preemies catch infections, common viruses, etc. You need to use more precaution.
What is A 25-26 Weeker’s NICU Stay Like?
A baby born at 25-26 weeks gestation weighs approximately 680-900 grams (1.5-2 pounds). At this gestation there is a survival rate of up to 80-90%.
Babies born at this gestation often require a breathing tube and ventilator. Some are quick to transition to a CPAP mask and then nasal cannula. Others will require long-term breathing support.
They’re unable to take feeds by mouth at this gestation. They will have IV lines placed. How long they’re dependent on IV based nutrition is unique to each baby.
They’ll eventually be given nutrition via an NG or OG tube (nasal or oral). Breast milk, whether yours or donor milk, is often fortified for babies at this gestation. The fortifier is preferably human milk-based fortifier for these very premature babies. An exclusive human milk diet reduces the risk of necrotizing fasciitis (NEC), a serious infection.
When breast milk is unavailable, they’re given formula designed to meet a preemie’s extra caloric and nutrient needs. NICUs use ready to feed formula which is sterile. Infection can still occur, but is less with sterile ready to feed compared to powdered formulas.
Exclusively pumping until baby can feed at the breast can be very time consuming and quite challenging. However, every drop you’re able to provide is important as it’s helpful for their development. It is also extremely helpful for preventing infection.
The earlier a baby is born, the higher their risk of chronic lung disease, developmental delays, and other long-term health conditions. For this reason, as mentioned above, it’s important to work with specialist pediatricians to keep an eye on their development.
How Long Are 27-28 Weeker’s in The NICU?
Babies born around 27-28 weeks need a good bit of support still. However, their respiratory system is more developed than at 23-26 weeks. A baby born at this gestation should expect a NICU stay close to their original due date.
A 27-28 weeker may or may not need support from a ventilator. They will need some respiratory support, however. It may be a ventilator, CPAP or nasal cannula. How long they need support varies greatly from baby to baby. Some quickly graduate to room air, while others will need long-term support.
Feeding guidelines vary from hospital to hospital. Your baby will likely have IV and umbilical lines placed for immediate nutrition, hydration, and medicine. They will also likely have an OG or NG tube.
Many facilities don’t start oral feedings (breast or bottle) until 32 to 34 weeks gestational age. This is because preemies aren’t yet able to safely suckle, swallow, and breath properly. Breastfeeding and bottle feeding can be very tiring for them, using up their little bit of energy quickly.
Using Skin-to-Skin
Skin to skin, also known as kangaroo care, is extremely beneficial for preemies. Depending on your baby’s level of life support, you may be able to hold them immediately. Sometimes you will need to wait a few days to a few weeks. Things such as an umbilical artery line make it dangerous to move baby. You can talk to your baby’s nurses about how you can provide positive touches even when baby cannot be picked up.
Getting to hold your baby for the first time can be exciting and simultaneously terrifying. The wires, tubes and breathing support can be overwhelming, but your baby’s nurse can help you get comfortable.
Babies born at this gestation are around 1000 grams or 2 pounds so with a bit of help, you’ll learn to easily navigate all the wires and tubes.
Many premature babies catch up in growth and development around 2-3 years of age. The earlier they’re born, the longer this can take. Of course, just as with full-term babies, every baby develops at their own unique pace. Do not compare your baby with any others, preemie or full-term.
Just like preemies born at 23-36 weeks, these babies will still be at an increased risk of developmental delays and chronic health conditions. It can be helpful to prepare for such circumstances while also remembering that a risk is not a guarantee. Many preemies thrive and do extremely well long-term.
What Is The NICU Like For 29-30 Weekers?
Babies born at 29-30 weeks gestation are still very premature and in need of a lot of medical support. However, their respiratory system, and other systems, are a bit more developed than their earlier preemie peers making them a bit less fragile.
A baby born around this time is about 1 kgs or 2.5 pounds. Some babies are much smaller due to conditions such as intrauterine growth restriction (IUGR), preeclampsia, or other things which can lead to preterm births.
Babies born at this gestation may or may not require a breathing tube (intubation) and ventilator. Some will require long-term breathing support; others are on room air within a few days or weeks.
They will not be ready for oral feeding for a few weeks and will require and NG or OG tube. They will also have IV lines placed for at least the first few days, longer dependent upon their nutrition and medical needs.
Preemies will have frequent blood sugar tests until the NICU team is sure they can maintain their blood sugar levels. This can be for just a day or two, or for several weeks. They will also have heel sticks to get a small amount of blood to check for jaundice. They may only need one to a few draws, or they may need several over the course of a few weeks.
If their bilirubin levels are high, they will receive phototherapy for jaundice. This is a non-invasive treatment. If you come in one day and see your baby’s bed looking blue, it’s simply phototherapy.
Every baby born before 34 weeks, and many born before 36, will spend some time in the NICU. The earlier a baby is born, the longer they are likely to be in the NICU. Many NICUs will tell parents to prepare for their baby to stay until their original estimated due date. Some will go home a bit before, others a bit after. Every baby is unique, of course, and their length of stay will vary.
What To Expect in The NICU With A 31-32 Weeker
A 31–32-week baby weighs around 1.5-2 kgs (3-4.5lbs). Their NICU experience is often similar to 27-30 weekers but they may go through each stage a little faster than their earlier preemie peers.
They are likely to have lees time on breathing support, less time with IVs, less time with a feeding tube, etc. Each week a baby remains in utero, the more developed every system is. Some of these babies will even be ready to go home around 35-37 weeks.
However, many will still need more time in the NICU to get their feeding skills down, reach a certain weight, outgrow apnea of prematurity, and maintain their body temperature.
Occasionally, babies are sent home with medical devices (e.g. apnea monitor, feeding tube, etc.,) but in most cases, the best situation is waiting for them to outgrow the need for any devices.
Some facilities will allow practice attempts at the breast or bottle at this gestation. Non-nutritive suckling happens now. However, many wait until 33-34 weeks to be safer.
Depending on their respiratory support, some babies will need to wait even longer as it’s unsafe to attempt oral feeds with certain devices in place.
What is The Stay Like?
Babies at this gestation will typically have an IV and/or umbilical lines placed at birth. This allows nutrition and medication to be given quickly. Doctors can also easily check their blood gases (ensuring they’re getting enough oxygen). Some babies won’t need IVs for very long, others may need them for a couple to several weeks.
The longer a baby develops in utero, the lower their risk of long-term developmental delays and medical conditions associated with prematurity. Being premature comes with risks, but each day in utero lowers the risks.
Your baby will be monitored in the NICU for signs of brain bleeds (less likely the longer they remain in utero, as well as when mothers receive magnesium before birth) which can be associated with developmental concerns. However, having a brain bleed does not always indicate future complications.
Premature babies should also be monitored after discharge until they catch up to their full-term peers (often by 2-3 years), or receive necessary support to help them develop their best at their own pace. Having developmental delays early in childhood does not always equal long-term complications. Early intervention helps premature infants reach each milestone in their best way, regardless of their own unique timeline.
What To Expect With A 33-34 Weeker
Most hospitals require every baby born under 35 weeks to at least be evaluated, if not admitted to the NICU. A 33 weeker will almost definitely require some time in the NICU. They are unlikely able to successfully breast or bottle feed full feedings at 33 weeks and may need time to learn to maintain their body temperature.
A 34 weeker, very occasionally, is discharged when her mother is discharged, but most need a bit of support transitioning after birth.
Some 33-34 weekers can breathe room air right away, but many will also need some respiratory support. While it’s possible they’ll need a ventilator, some need a CPAP, and many only a nasal canula.
For many 33-34 weekers, the biggest challenges are oral feeding, jaundice and maintaining body temperature.
These babies are more likely to be discharged prior to their original due date. However, it’s still a good idea to be prepared for a 6-7 week stay. It’s possible your baby may need more time to meet discharge requirements.
Do 35-36 Weekers Go To The NICU?
Many babies at this gestation will need some monitoring while in the hospital to be sure they’re transitioning and feeding well.
Some 35-36 weekers will need some time in the NICU to learn to feed and maintain their body temperature. Occasionally, some require respiratory support. Some 35-36 weekers are discharged with their mother. Others will need a few days to a few weeks in the NICU.
The near term preemies are more likely to have some feeding difficulties as they’re less alert than their full-term peers. They’re also more likely to need phototherapy for jaundice, and they may require blood sugar monitoring.
A 35-36 weeker often weighs around 2.2-2.7 kgs (5-6lbs). Some are much bigger and closer to a full-term baby size. Others are much smaller when IUGR, preeclampisa, etc. are involved.
Many babies at this gestation quickly catch up to their full-term peers and rarely need to account for adjusted age in the same way an earlier preemie would need to. That said, every day and week in utero is extremely beneficial for development. They’re still at an increased risk of needing early intervention support (e.g. physical, speech or occupational therapy) when compared to their full-term peers. Keeping track of development and following up as needed is important.
Having a preemie can be scary and overwhelming. It’s rarely expected and it’s certainly not the desired outcome for a pregnancy. Fortunately, with modern neonatology and many early intervention specialists, preemies today not only survive, but most also thrive quite well!
If you are expecting or already have a preemie, be sure to reach out to Today is a Good Day for support, NICU related podcasts, and more!